Among 19 patients assessed for gastric and bowel function, 8 (42%) had impaired ability to move food from the esophagus to the stomach, with 2 of these 8 reporting difficulty swallowing. Thirteen of 18 patients (72%) had impaired eating and digestive function, including self-reported dysphagia. Ten of 16 patients (63%) had lower maximum inspiration pressures, indicating weakness of the muscles involved in breathing. Thoracic ultrasound showed flattened diaphragmatic curves, indicating abnormal breathing, in 10 participants (46%). Ultrasound examination revealed that at 6 (27%) had alterations of the vagus nerve in the neck, including thickening of the nerve and increased echogenicity, which indicates mild inflammatory changes. Nineteen of 22 participants (86%) had three or more VND symptoms with a median duration of 14 months. The most common VND symptoms were diarrhea (73%), tachycardia (59%), dizziness, dysphagia and dysphonia (45% each), and orthostatic hypotension (14%). The ongoing study involved the first 22 participants identified as having at least one VND symptom 91% of them were women, and the median age was 44 years. Of the 348, 228 (66%) had at least one symptom that could be attributed to vagus nerve dysfunction (VND). In the observational study, the researchers evaluated the morphologic and functional aspects of the vagus nerve in 348 patients diagnosed as having long COVID at a Spanish hospital from March to June 2021. Long COVID has been reported to last for months to more than a year. 
The study authors said that SARS-CoV-2 infection may lead to long COVID symptoms such as dysphonia (voice problems), dysphagia (difficulty swallowing), dizziness, tachycardia (rapid heart rate), orthostatic hypotension (low blood pressure), and diarrhea. It has a role in heart rate, speech, the gag reflex, the transfer of food from the mouth to stomach, transporting food through the intestines, perspiration, and other bodily functions. The vagus nerve runs from the brain into the torso, heart, lungs, intestines, and several muscles, including those involved in swallowing. 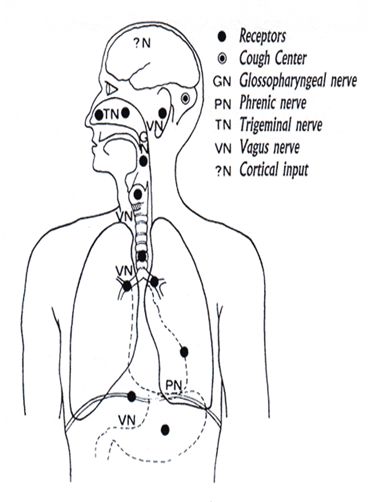
Long COVID, vagus nerve symptoms may overlapĪt the European Congress of Clinical Microbiology and Infectious Diseases (ECCMID), slated for Apr 23 to 26 in Lisbon, Portugal, a team led by researchers in Spain will discuss the role of the vagus nerve in long COVID, according to an ECCMID news release. Neither study has been peer-reviewed, and the second one comes with the added caveat that it was conducted by an EECP provider. Long COVID may affect up to 15% of those who survive their infections, causing symptoms such as fatigue, muscle pain, and cognitive problems that linger for months. Two studies to be presented at upcoming professional society meetings suggest that some long COVID-19 symptoms may be related to the effect of SARS-CoV-2 on the vagus nerve and that the use of enhanced external counterpulsation (EECP)-which increases blood flow-can improve some of those symptoms, respectively. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
